Preliminary Findings From the Saint Thomas Strong Study
Publication Date: 2018
Abstract
Children who experience natural disasters are at risk of developing symptoms of post-traumatic stress disorder (PTSD), anxiety, and depression. In this study, 109 children in Grades 3–12 were recruited from private and public schools on the island of Saint Thomas in the U.S. Virgin Islands, where two Category 5 hurricanes hit in September 2017. Three months after the hurricanes, participants completed questionnaires that asked about their experiences during and after the hurricanes, their social support, the use of various coping strategies, and their current psychological functioning. Almost half (47 percent) of the children reported moderate or severe levels of PTSD symptoms, with 24 percent reporting clinically meaningful levels of internalizing symptoms (i.e., symptoms of anxiety and depression). At a trend level, children who experienced more life-threatening experiences, but not loss-disruption experiences, were found to have more PTSD symptoms. Children with higher levels of PTSD symptoms reported lower levels of social support from parents, teachers, and their schools, but no link was found to social support from friends. In addition, the use of several coping strategies (e.g., distraction, social withdrawal, and problem-solving) was associated with higher levels of PTSD. Only cognitive restructuring and mindfulness were linked with lower levels of PTSD.
Background and Research Questions
Children and adolescents who are exposed to traumatic events are at risk of developing a wide variety of negative psychological outcomes, including traumatic stress, depressive symptoms, and anxiety (Trickey et al. 20121). While the vast majority of individuals who experience natural disasters experience some symptoms in the first few weeks after the event, those who continue to struggle two to three months after the disaster are at risk of long term difficulties (La Greca and Silverman 20092). This study focuses on understanding what factors contribute to worse functioning in children in this early recovery phase, which influences who will do better over time.
Previous research has shown that experiencing a Category 5 hurricane is a traumatic event that is associated with these difficulties. For example, three months after Hurricane Andrew hit Florida in 1992, 56 percent of third, fourth, and fifth graders reported moderate to severe symptoms of PTSD; while these rates declined over the year, 34 percent continued to have elevated symptoms 10 months after the event (La Greca et al. 19963). Understanding what factors either positively or negatively influence children’s psychological outcomes in the aftermath of a natural disaster is an important question that can inform how to identify children most at risk, as well as what interventions may lead to more positive outcomes in children over time.
Several factors can increase the likelihood that children and adolescents will experience symptoms of traumatic stress after a hurricane or other natural disaster. These include the degree of exposure during the traumatic event and the severity of impact after the event (e.g., damage to homes and the need to relocate; La Greca et al 1996). In addition, several demographic variables have been suggested as influential in predicting children’s responses in a recent meta-analysis. Specifically, children who are female and younger (at least when the trauma is experienced by a group, such as in a hurricane), and who have few family resources are more likely to have increased levels of post-traumatic stress (Trickey et al. 2012).
In contrast to the number of studies focused on the identification of risk factors, few have considered what may lessen the likelihood of negative outcomes in the aftermath of a natural disaster (i.e., protective factors). One study has found that children fare better when they perceive higher levels of social support (Vernberg et al 19964). However, previous research has only examined social support as a larger composite and has not considered the source of the support. While parents and friends are likely sources, teachers and the school may also be important sources of social support (e.g., Atkins et al. 20175). Thus, this study examines multiple sources of social support, including parents, friends, teachers, and schools to see if their impact on children’s functioning varies.
In addition to social support, the use of more effective coping strategies is another possible factor that has been found to be important when examining children’s responses to stressors (Compas et al. 20016). However, models of coping are numerous, and the effectiveness of a coping strategy may vary based on the type of stressor faced (see Compas et al. 2001 for a review). Models include examining primary versus secondary control (i.e., focusing on changing the event as opposed to adapting to the event; Adamson and Thompson 19987); problem-focused versus emotion-focused coping (e.g., Picci et al. 20158), and coping focused on engagement as compared to disengagement with the event (e.g., Evans et al. 20159). Because these models are overlapping and often contradictory (Compas et al. 2001), rather than considering these larger level constructs, this study focuses on the specific coping strategies used to explore what may be helpful or potentially harmful to children who have experienced natural disasters. These include the use of distraction, social withdrawal, cognitive restricting, self-criticism, blaming others, problem-solving, emotion regulation, wishful thinking, social support, resignation, and prayer.
In addition to these commonly considered coping strategies, in recent years, the clinical literature has focused on the possible impact of mindfulness on psychological functioning in children and adolescents (e.g., Harnett and Dawe 201210); however, its impact on symptoms of PTSD has only been considered among adults (e.g., Thompson, Arnkoff, and Glass 20111). Mindfulness is the act of being aware of the moment-to-moment experiences in one’s life with acceptance and no judgment, and may be particularly helpful in the aftermath of an event that individuals cannot control. Thus, children’s degree of mindfulness will be considered as an additional coping strategy that may be protective in the aftermath of a hurricane.
In summary, there are multiple risk and protective factors that may influence the well-being of children in the aftermath of a hurricane. Given that experiencing a hurricane is considered a trauma, symptoms of PTSD were a primary outcome considered. In addition, internalizing symptoms (including symptoms of anxiety and depression) were considered, as they have been found to be linked to experiencing natural disasters. Finally, externalizing symptoms, which include “acting out” behaviors associated with oppositional defiant disorder and conduct disorder, were also examined. While previous research has not reported elevations in children’s externalizing behaviors in the aftermath of hurricanes, it was hoped that an assessment of these symptoms might show a differential pattern of influence that would indicate specific impacts on PTSD and internalizing symptoms, but not externalizing symptoms. Thus, in this study, the following research questions were asked:
1) What experiences during and after the hurricane were associated with negative psychological outcomes? 2) What demographic (i.e., age, gender, ethnicity), individual (i.e., coping strategies used), and relational (i.e., social support from parents, friends, teachers, and the school) factors contribute to better functioning of children and adolescents who have experienced a natural disaster?
Method
Sample
Children in grades 3–12 (n = 109) were recruited from schools on Saint Thomas three months after two Category 5 hurricanes—Irma and Maria—hit the island within weeks of each other. Children were 56 percent female (44 percent male) and primarily Afro-Caribbean (75 percent). The sample included 47 percent who were enrolled in public elementary schools, 38 percent who were enrolled in a public junior high, 7 percent who were in a specialized public high school, 6 percent who were in a private high school, and 3 percent who were homeschooled (mean age = 11.4 years [standard deviation (SD) = 2.53 years]). These schools were selected to provide a sample with a range in family socioeconomic status, ethnicity, and the impact that the hurricanes had on the school and home environments.
Procedures and Measures
Children in grades 3–12, with parental consent, were asked to complete electronic surveys during the school day. These were completed on handheld devices provided by the research team using Qualtrics offline. Children were asked about their:
- backgrounds
- current grades
- symptoms of PTSD using the UCLA Reaction Index (Steinberg et al. 201312),
- other psychological symptoms (e.g., depression, anxiety, or acting out behaviors) using the Pediatric Symptom Checklist (Jellinek et al. 199913)
- exposure to and loss after the hurricanes using the Hurricane-Related Traumatic Experiences Questionnaire (Vernberg et al. 1996)
- perceived social support from parents, teachers, close friends, and the school using the Child and Adolescent Social Support Scale (Malecki and Demaray 200214)
- coping strategies used based on reports in the KidCope questionnaire (Spirito, Stark and Knapp 199215).
Each child was given several small gifts for his or her participation, including a Saint Thomas Strong wristband, candy, and a gel pen.
Results
Descriptive Statistics
The vast majority (94 percent) of the child participants were on the island for both Hurricanes Irma and Maria; only two participants were not on the island for both hurricanes. Table 1 provides the percent of participants who experienced specific negative and/or scary events during the hurricanes. As indicated, 39 percent of participants thought they might die during the hurricane and 35 percent had windows or doors broken during the events. About a quarter of the sample had their homes badly damaged, though only 6 percent moved as a result. In addition, a third of the participants indicated that they had trouble getting enough food or water after the hurricanes. The most common disruption reported was trouble seeing friends who had moved away.

Table 1. Percent of participants who experienced specific events during and after the hurricanes
Table 2 provides descriptive statistics for all measures. As discussed, most participants had been on the island during at least one hurricane. On average, participants had experienced at least one life-threatening event during the hurricanes. In addition, participants experienced, on average, almost two losses or disruptions to their lives. The severity of psychological symptoms varied across the sample. While 53 percent of participants reported a low level of PTSD symptoms (i.e., met criteria in one or fewer of the needed Diagnostic and Statistical Manual of Mental Disorders (DSM) domains), 35 percent reported a moderate level of PTSD symptoms (i.e., met criteria in two or three of the needed DSM domains), and 12 percent were at high risk for PTSD, meeting the criteria in all four of the DSM domains needed for diagnosis. These levels are fairly consistent with those reported in previous research with children three months after a hurricane (La Greca et al. 1996). Many children also reported symptoms that were above suggested clinical cutoffs for internalizing symptoms (24 percent), with only 6 percent reporting symptom levels above clinical cutoffs for externalizing symptoms. This supports previous findings that suggest that experiencing a hurricane influences internalizing, and not externalizing, problem behaviors (Goenjian et al. 200116).
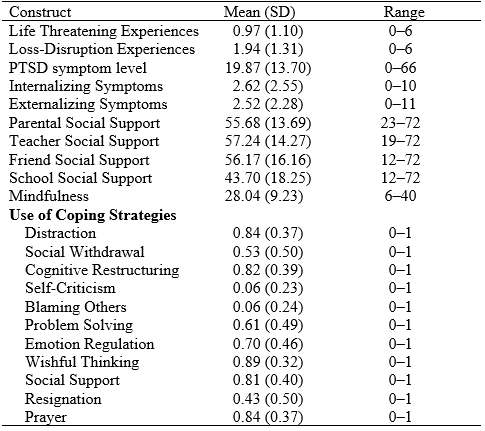
Table 2. Descriptive statistics
Table 2 also reports the percent of children who used multiple coping strategies in order to handle the stress experienced after the hurricanes. The most commonly used strategies were wishful thinking (89 percent), distraction (84 percent), prayer (84 percent), cognitive restructuring (82 percent), and social support (81 percent). Less commonly used strategies were self-criticism (6 percent) and blaming others (6 percent).
Associations with Psychological Functioning
Individual Characteristics. In contrast to previous studies (e.g., Trickey et al., 2012), PTSD symptoms were not correlated with age (r = -.13, p = .19); however, grade was negatively correlated (r = -.22, p = .02), and participants in higher grades reported fewer PTSD symptoms. Neither grade nor age was associated with other psychological symptoms. In addition, t-tests found no significant differences by child gender when examining all psychological symptoms (i.e., PTSD, internalizing, and externalizing symptoms). Similarly, using analysis of variance (ANOVA) procedures, no significant differences were found in psychological outcomes based on ethnic group.
Hurricane-related experiences. A series of t-tests were run to examine whether there were differences in symptom levels based on experiencing specific events during and after the hurricanes. Participants who reported thinking that they might die during the hurricanes had more PTSD symptoms (mean = 23.18 [SD= 13.41]) compared to those who did not think they would die (mean = 17.37 [SD= 13.41], t = -2.143, p = .035). Similarly, those who thought they would die had more internalizing symptoms (mean = 3.44 [SD = 2.87]) compared to those who did not think they would die (mean = 2.08 [SD = 2.22] , t = -2.63, p = .01). No differences were found for externalizing symptoms. In addition, symptom levels were not found to vary based on the experience of any other specific event during or after the hurricanes.
To determine if the number of life-threatening experiences during the hurricanes or the degree of disruption after the hurricanes were linked to psychological functioning, composite scores were created that summed the number of events experienced. As shown in Table 3, the more negative experiences that a child had during the hurricanes were associated with higher levels of PTSD symptoms at a trend level, but not with other types of psychological functioning. Experiences of loss and disruption after the hurricanes were not associated with any of the symptoms assessed.
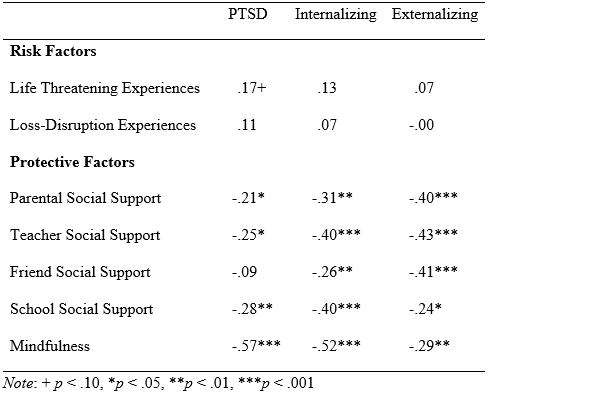
Table 3. Bivariate Correlations Between Risk and Protective Factors and Symptom Outcomes
Social Support. As shown in Table 3, most types of social support were negatively associated with psychological functioning in this sample. Greater reports of social support from parents, teachers, friends, and the school were linked to lower levels of externalizing and internalizing behaviors, suggesting an overall positive impact of social support on children’s mental health. While parent, teacher, and school social support were associated with lower levels of PTSD symptoms, friend social support was not significantly associated. This suggests that in response to the hurricanes, friends are not an adequate support system, perhaps because they also are experiencing significant distress. In addition, the findings suggest that children’s psychological functioning is linked to their relationships with teachers and the school, as well as with their parents.
Coping Strategies. As shown in Table 3, mindfulness was strongly associated with lower levels of PTSD and other psychological symptoms. Given this coping strategy has not been assessed in previous studies examining children’s functioning in the aftermath of a hurricane, this suggests the need for further study.
In considering the use of other more traditional coping strategies, a series of t-tests were run, comparing children who used a strategy versus those who had not used the strategy. As shown in Table 4, children had higher levels of PTSD symptoms when they used the following coping strategies: distraction, social withdrawal, self-criticism (at a trend level), problem-solving, and emotion regulation. While several of these coping strategies are seen as ineffective, problem-solving and emotion regulation may be expected to be positively related to psychological functioning. However, in the face of events that cannot be controlled, problem solving may not be an effective strategy, leading to more frustration. In addition, it may be that those who are experiencing the greatest level of distress are trying to use multiple coping strategies but not successfully. It should be noted that cognitive restructuring (i.e., “I tried to see the good side of things”) was the one coping strategy associated with a lower number of PTSD symptoms, suggesting that it is the most useful coping strategy.
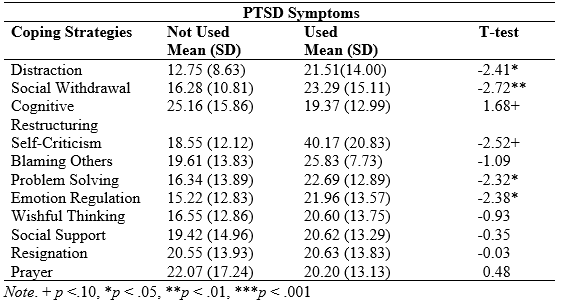
Table 4. T-Tests of the Use of Coping Strategies Predicting PTSD
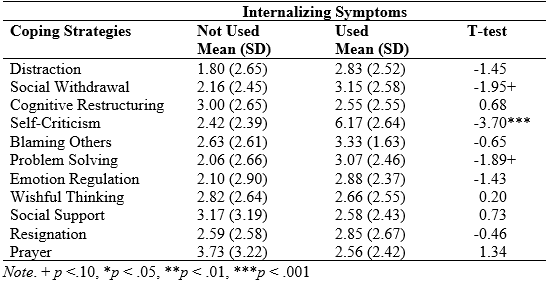
Table 5. T-Tests of the Use of Coping Strategies Predicting Internalizing Symptoms
As shown in Table 5, fewer coping strategies were associated with internalizing symptoms. Children who used self-criticism (i.e., “I blamed myself for causing the problem”) had significantly more internalizing symptoms than those who did not. In addition, at a trend level, children who used social withdrawal and problem solving had higher levels of internalizing symptoms. While social withdrawal is strongly linked with depressive symptoms, like with PTSD, problem solving (e.g., “I tried to fix the problem by thinking of answers”) may lead to greater frustration, as the events related to the hurricane are outside the child’s control.
While the number of participants who exhibited high levels of externalizing symptoms were not as great as those who exhibited internalizing or PTSD symptoms, the use of social withdrawal and self-criticism were both associated with more externalizing symptoms (see Table 6), similar to their associations with internalizing symptoms. Unexpectedly, the use of wishful thinking was linked to lower levels of externalizing symptoms.
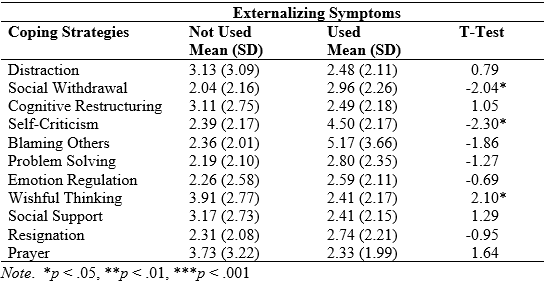
Table 6. T-Tests of the Use of Coping Strategies Predicting Externalizing Symptom
Applications of Findings
This study suggests that children and adolescents experience similar negative psychological consequences after a hurricane, with almost half experiencing moderate or severe levels of PTSD. Many also experience clinically significant levels of internalizing symptoms. The link to externalizing symptoms is less evident. Thus, the development of strategies to target the reduction of symptoms is needed. While cross-sectional in design, the findings from this study suggest that social support from parents, teachers, and schools, and certain types of coping strategies (i.e., mindfulness and cognitive restructuring) may be particularly helpful in the aftermath of experiencing two hurricanes. Thus, interventions that aim to increase social support from parents or teachers may be particularly useful. In addition, the use of cognitive strategies that help children reframe events they have experienced may be helpful and may help children understand how positive outcomes can result from tragedies. Finally, teaching children how to be more mindful may also be helpful in symptom reduction. Given the rising interest in the use of mindfulness-based interventions with children and families more broadly (e.g., Harnett and Dawe 2012), this may be a promising intervention to test with individuals who have experienced natural disasters.
Future plans
Though beyond the scope of this report of preliminary findings, additional data was collected in this study that focused on the teachers in the elementary schools. Specifically, 28 teachers completed measures reporting their background characteristics, PTSD symptoms according to the PTSD Checklist for DSM-5 (Weathers et al. 201317), and psychological symptoms using the Depression Anxiety Stress Scales (Lovibond and Lovibond 199518). In addition, the teachers reported on the school and on the social competence and psychological symptoms of children in their classrooms who had parental consent (69 students). Additional analyses will be run to examine how teachers’ experiences with the hurricanes and their subsequent psychological symptoms may have impacted the children in their classrooms.
Additional analyses with the child sample will also be run to determine whether the influence of the individual and relational factors on children’s psychological functioning vary by children’s age, gender, and ethnicity. For example, some work suggests that younger children are more negatively influenced by these traumatic experiences, and types of support may be more important to them (Trickey et al. 2012). In addition, age may influence the effectiveness of certain coping strategies.
Finally, while the initial response rate was lower than anticipated, the schools are interested in gathering more information on their students. Thus, the data collection team will return six months after the first time point to gather information from these same students to determine the developmental trajectory of their symptoms, as well as which of the factors explored may influence that trajectory. In addition, data from a larger sample of students will be gathered in these schools nine months after the hurricanes.
References
-
Trickey, David, Andy P. Siddaway, Richard Meiser-Stedman,Lucy Serpell, and Field, Andy P. 2012. “A meta-analysis of risk factors for post-traumatic stress disorder in children and adolescents.” Clinical Psychology Review 32: 122-138. ↩
-
La Greca, Annette M., and Wendy K. Silverman 2009. “Treatment and prevention of posttraumatic stress reactions in children and adolescents exposed to disasters and terrorism: What is the evidence?” Child Development Perspectives 3 (1): 4-10. ↩
-
La Greca, Annette M.,Wendy K. Silverman, Eric M. Vernberg, and Mitchell J. Prinstein. 1996. “Symptoms of posttraumatic stress in children after Hurricane Andrew: A prospective study.” Journal of Consulting and Clinical Psychology 64 (4): 712-723. ↩
-
Vernberg, Eric M., Annette M.La Greca, Wendy K. Silverman, and Mitchell J. Prinstein. 1996. “Prediction of posttraumatic stress symptoms in children after Hurricane Andrew.” Journal of Abnormal Psychology 105 (2): 237-248. ↩
-
Atkins, Marc S., Elise Cappella, Elisa S. Shernoff,Tara G.Mehta,and Erika L. Gustafson. 2017. “Schooling and children's mental health: Realigning resources to reduce disparities and advance public health.” Annual Review of Clinical Psychology 13: 123-147. ↩
-
Compas, Bruce E., Jennifer K. Connor-Smith, Heidi Saltzman, Alexandra H. Thomsen, and Martha E. Wadsworth. 2001. “Coping with stress during childhood and adolescence: Progress, problems, and potential.” Psychological Bulletin 127 (1): 87–127. ↩
-
Adamson, Jackie L., and Ross A. Thompson. 1998. “Coping with interparental verbal conflict by children exposed to spouse abuse and children from nonviolent homes.” Journal of Family Violence 13 (3): 213-232. ↩
-
Picci, Rocco L., Francesco Oliva, Federica Trivelli, Claudio Carezana, Marco Zuffranieri, Luca Ostacoli, Pier M. Furlan and Roberto Lala. 2015 “Emotional burden and coping strategies of parents of children with rare diseases.” Journal of Child and Family Studies 24 (2):514-522. ↩
-
Evans, Lindsay D., Chrystyna Kouros, Sarah A. Frankel, Elizabeth McCauley, Guy S. Diamond, Kelly A., Schloredt, and Judy Garber 2015. “Longitudinal relations between stress and depressive symptoms in youth: Coping as a mediator.” Journal of Abnormal Child Psychology 43 (2): 355-368. ↩
-
Harnett, Paul H., and Sharon Dawe. 2012. “Review: The contribution of mindfulness-based therapies for children and families and proposed conceptual integration.” Child and Adolescent Mental Health 17(4): 195-208. ↩
-
Thompson, Rachel W., Diane B. Arnkoff, and Carol R. Glass. 2011. “Conceptualizing mindfulness and acceptance as components of psychological resilience to trauma.” Trauma, Violence, & Abuse 12 (4): 220-235. ↩
-
Steinberg, Alan. M., Melissa J. Brymer, Soeun Kim, Ernestine C. Briggs, Chandra G. Ghosh, Sarah H. Ostrowski,Kevin J. Gulley, K., and Robert S. Pynoos. (2013). “Psychometric properties of the UCLA PTSD Reaction Index: Part 1.” Journal of Traumatic Stress 26: 1-9. ↩
-
Jellinek, Michael. S, J. Michael Murphy, Michelle Little, Maria E. Pagano, Diane M. Comer, and Kelly J. Kelleher. 1999. “Use of the Pediatric Symptom Checklist to screen for psychosocial problems in pediatric primary care: A national feasibility study.” Archives of Pediatric and Adolescent Medicine 153: 254 – 260. ↩
-
Malecki, Christine K., and Michelle K. Demaray. 2002. “Measuring perceived social support: Development of the child and adolescent social support scale.” Psychology in the Schools 39 (1): 1–18. ↩
-
Spirito, Anthony, Lori J. Stark, and Leonora G. Knapp.1992. “The assessment of coping in chronically ill children: Implications for clinical practice.” In Stress and coping in child health, edited by Annette M. La Greca, Lawrence J. Siegel, Jan L. Wallander, & C. Eugene Walker, 327-344. New York: Guilford Press. ↩
-
Goenjian, Armen K., Luis Molina, Alan M. Steinberg, Lynn A.Fairbanks, Maria L. Alvarez, Haig A. Goenjian, and Robert S. Pynoos. 2001. “Postraumtic stress and depressive reaction among Nicaraguan adolescents after Hurricane Mitch.” American Journal of Psychiatry 158 (5): 788-794. ↩
-
Weathers, F. W., B. T. Litz, T. M. Keane, P. A. Palmieri, B. P. Marx, and P. P. Schnurr. 2013. “The PTSD Checklist for DSM-5 (PCL-5) – Standard [Measurement instrument]. “https://www.ptsd.va.gov/professional/assessment/adult-sr/ptsd-checklist.asp ↩
-
Lovibond, Sydney H., and Peter S Lovibond. 1995. Manual for the Depression Anxiety Stress Scales. (2nd. Ed.) Sydney: Psychology Foundation. ↩
Pittman, L. (2018). Preliminary Findings from the Saint Thomas Strong Study (Natural Hazards Center Quick Response Research Report Series, Report 276). Natural Hazards Center, University of Colorado Boulder. https://hazards.colorado.edu/quick-response-report/preliminary-findings-from-the-saint-thomas-strong-study